
Interstitial Lung Disease (ILD)
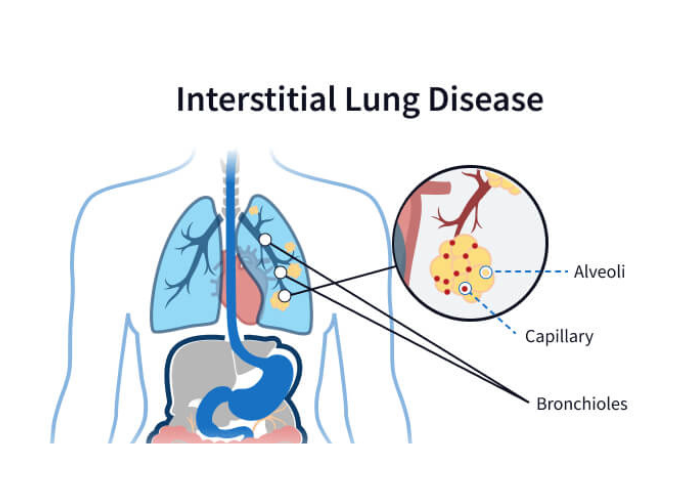
Interstitial Lung Disease (ILD) is a group of lung disorders that cause progressive scarring (fibrosis) of the lung tissue, particularly the interstitium, which is the tissue around the air sacs. This scarring makes it difficult for oxygen to pass into the bloodstream, leading to breathing difficulties and reduced oxygen levels. ILD can result from long-term exposure to environmental pollutants, occupational hazards, autoimmune diseases, certain medications, or may be idiopathic (unknown cause). Common symptoms include persistent dry cough, shortness of breath, fatigue, and chest discomfort. Early diagnosis and management are crucial to slow disease progression and improve quality of life.
Diagnosis usually involves a combination of chest X-rays, high-resolution CT scans, pulmonary function tests, blood tests, and sometimes lung biopsy. Treatment focuses on reducing inflammation, managing symptoms, and slowing disease progression. Supportive therapies, lifestyle changes, and sometimes surgical interventions like lung transplantation may be necessary in severe cases. Regular monitoring and follow-up with a pulmonologist are essential to prevent complications and maintain lung function.
Care & Management of Interstitial Lung Disease (ILD)
- Avoid smoking and secondhand smoke
- Limit exposure to pollutants, dust, and chemicals
- Regular monitoring of lung function
- Pulmonary rehabilitation and breathing exercises
- Stay hydrated and maintain nutrition
- Vaccinations: flu, pneumonia
- Manage underlying autoimmune or related conditions
- Oxygen therapy if required
- Regular follow-up with a pulmonologist
- Take prescribed anti-inflammatory or antifibrotic medications
Treatment of Interstitial Lung Disease (ILD)
1. Medications:
2. Supportive Care:
3. Surgical Options:
Frequently asked questions
Causes include autoimmune diseases, long-term exposure to toxins, medications, infections, or idiopathic (unknown cause).
Most forms cannot be fully cured, but treatments can slow progression and manage symptoms.
Persistent dry cough, shortness of breath, fatigue, chest discomfort, and sometimes clubbing of fingers.
Through imaging (X-ray, HRCT), pulmonary function tests, blood tests, and sometimes lung biopsy.
