
Sleep Apnea
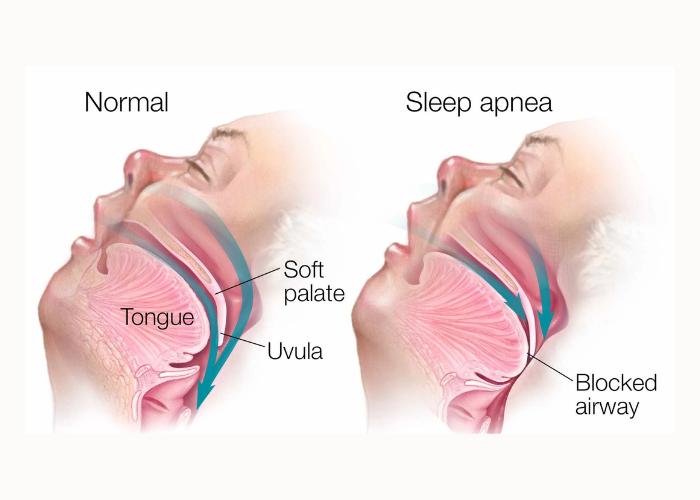
Sleep apnea is a sleep disorder characterized by repeated interruptions in breathing during sleep. These pauses can last from a few seconds to over a minute and may occur dozens of times per night. There are three main types: obstructive sleep apnea (OSA), caused by airway blockage; central sleep apnea (CSA), caused by the brain failing to signal breathing muscles; and complex (mixed) sleep apnea, a combination of both. Common symptoms include loud snoring, daytime sleepiness, morning headaches, difficulty concentrating, and restless sleep. Untreated sleep apnea can increase the risk of high blood pressure, heart disease, stroke, diabetes, and impaired cognitive function.
Diagnosis of sleep apnea involves a detailed sleep history, physical examination, and a sleep study (polysomnography) to monitor breathing patterns, oxygen levels, and heart activity during sleep. Early diagnosis and treatment are crucial to prevent long-term complications and improve quality of life. Lifestyle modifications, medical devices, and sometimes surgery can help manage sleep apnea effectively.
Care & Management of Sleep Apnea
- Weight management
- Avoid alcohol & sedatives before bedtime
- Sleep on side instead of back
- Maintain regular sleep schedule
- Treat nasal congestion or allergies
- Use CPAP or BiPAP devices (for OSA)
- Oral appliances to keep airway open
- Avoid smoking
- Monitor blood pressure and heart health
- Follow-up with sleep specialist regularly
Treatment of Sleep Apnea
1. Lifestyle Changes:
2. Medical Devices:
3. Surgery (if needed):
4. Monitoring & Follow-up:
Frequently asked questions
Loud snoring, daytime sleepiness, morning headaches, difficulty concentrating, restless sleep.
Obstructive sleep apnea can often be managed effectively with lifestyle changes, devices, or surgery, but ongoing management may be needed.
Through a sleep study (polysomnography) and physical examination.
Yes, if untreated, it increases the risk of heart disease, stroke, diabetes, and accidents due to daytime sleepiness.
