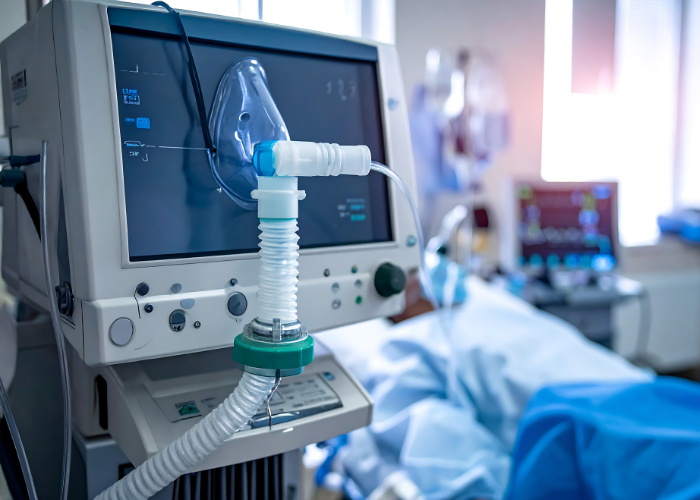
Ventilator Management
Ventilator management refers to the medical care and monitoring of patients who require mechanical ventilation to support or replace normal breathing. Ventilators are commonly used in critically ill patients with respiratory failure due to conditions such as severe pneumonia, ARDS, COPD exacerbations, neuromuscular disorders, trauma, or post-surgical complications. Proper ventilator management ensures adequate oxygen delivery, removal of carbon dioxide, and reduced work of breathing while minimizing lung injury.
Effective ventilator management involves selecting appropriate ventilator modes, adjusting settings based on patient condition, and continuous monitoring of respiratory parameters. The goal is to support the lungs while promoting recovery and timely weaning from ventilation. Multidisciplinary care involving pulmonologists, intensivists, respiratory therapists, and nursing staff is essential to optimize outcomes and reduce complications such as ventilator-associated pneumonia or lung injury.
Care & Management in Ventilator Management
- Select appropriate ventilator mode
- Optimize oxygen concentration and tidal volume
- Maintain airway hygiene and suctioning
- Monitor oxygen saturation and blood gases
- Prevent ventilator-associated pneumonia (VAP)
- Ensure proper sedation and comfort
- Regular assessment for weaning readiness
- Maintain head-end elevation
- Monitor for pressure injuries and barotrauma
- Continuous multidisciplinary monitoring
Uses & Importance of Ventilator Management
1. Respiratory Support:
2. Critical Care:
3. Recovery & Monitoring:
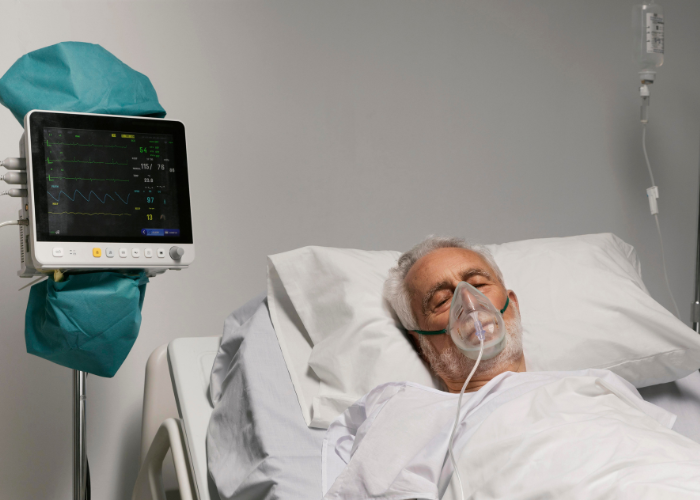
Frequently asked questions
Medical supervision and adjustment of mechanical ventilation to support breathing in critically ill patients.
Patients with severe breathing failure due to lung, heart, neurological, or critical illnesses.
No, most patients are supported temporarily until they recover and can breathe independently.
Ventilator-associated pneumonia, lung injury, airway irritation, muscle weakness.
